I’ve had quite a few questions about COVID-19 put to me by friends and family members recently, and so last week I had intended to begin trying my best to answer them. This plan had to be put on hold when Waco (and various other cities in Texas) issued a requirement to wear a face mask inside of businesses and restaurants, and the whole world sort of lost it’s collective mind. I think things have calmed down now, at least locally, and as I’ve driven to clinic and back and the one or two other places I couldn’t really avoid going, I’ve thankfully seen a noticeable increase in masking, either in compliance with this decision or in response to the efforts of so many to share reliable information on the benefits and safety of wearing a face mask. Thank you all for fighting the crazy amount of misinformation out there. For my take on wearing masks you can read my previous blog post on masking.
Now in 8-bit Color!
Now that we’ve made it through another week without another viral misinformation video, I’m finally taking the time to sit down and write that original post I had planned on. I’ve tried to limit myself to just two paragraphs for each topic (paragraph length unspecified), but given just how many questions
Due to length, I’ve broken this post up into multiple parts.
Warning: These got really ‘mathy’ on me before I realized it was happening.
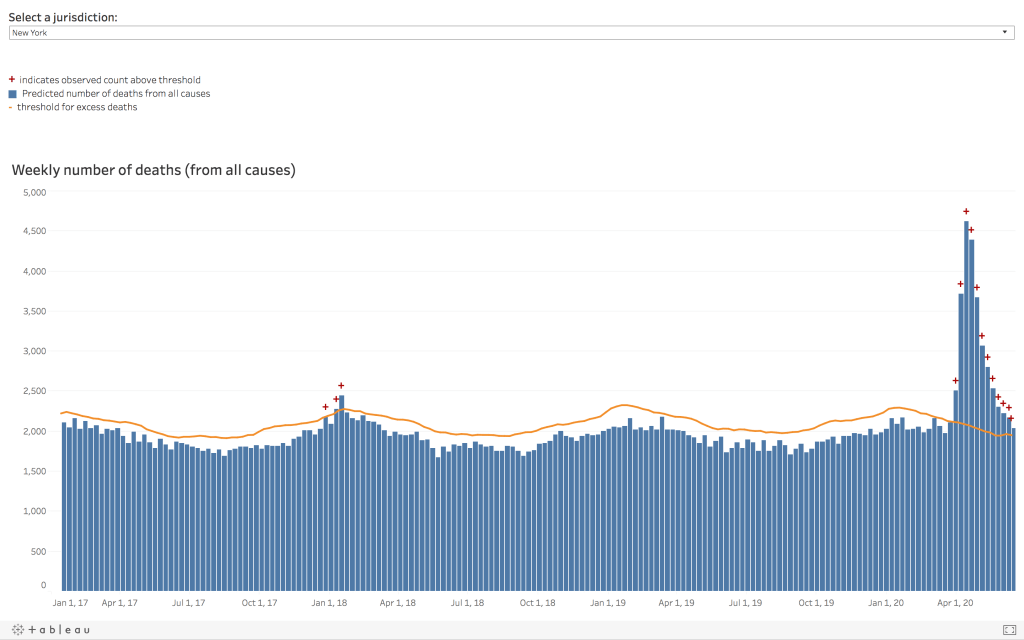
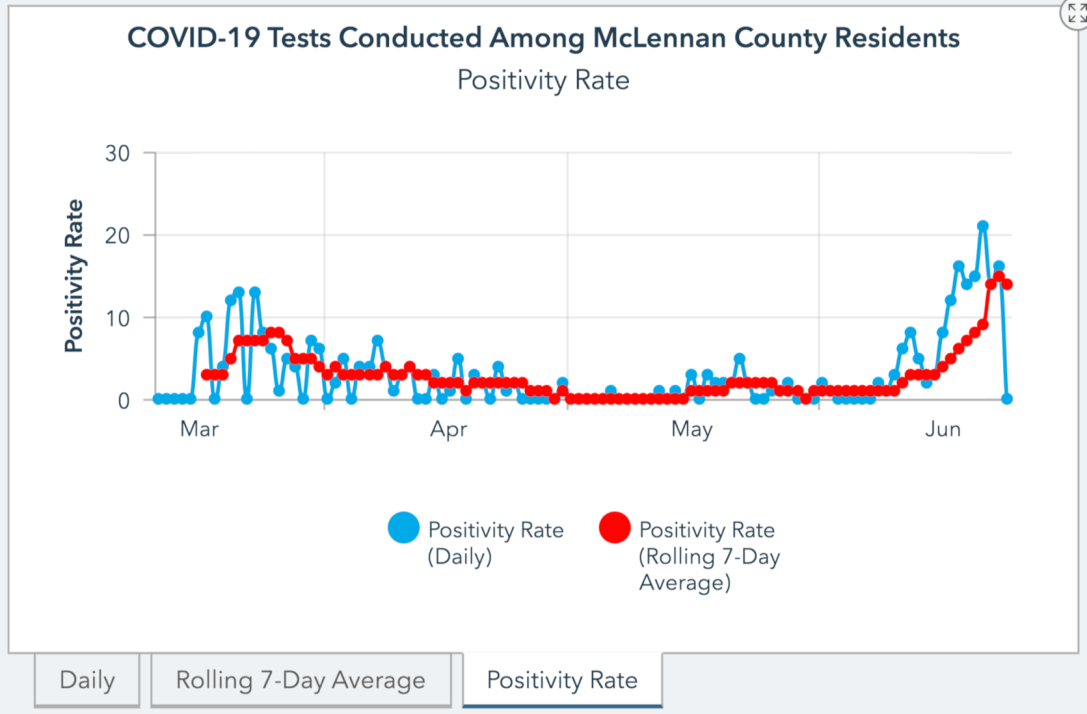
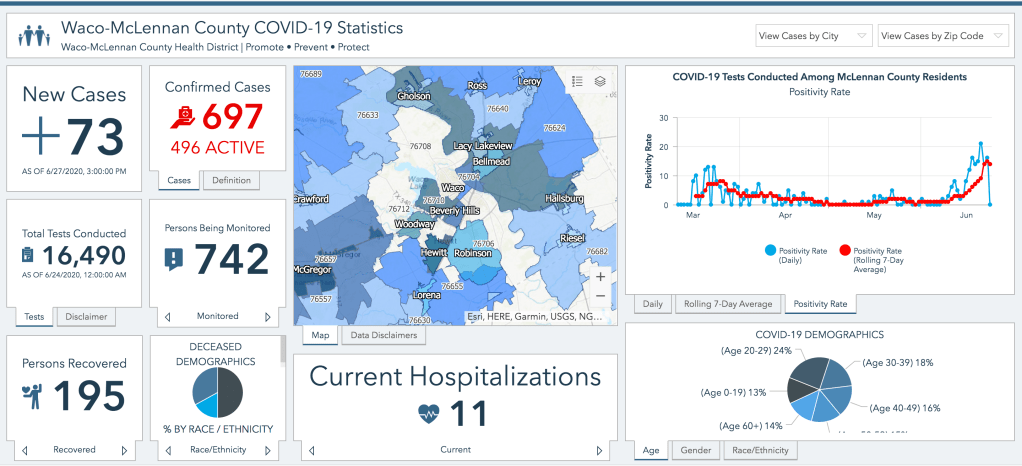
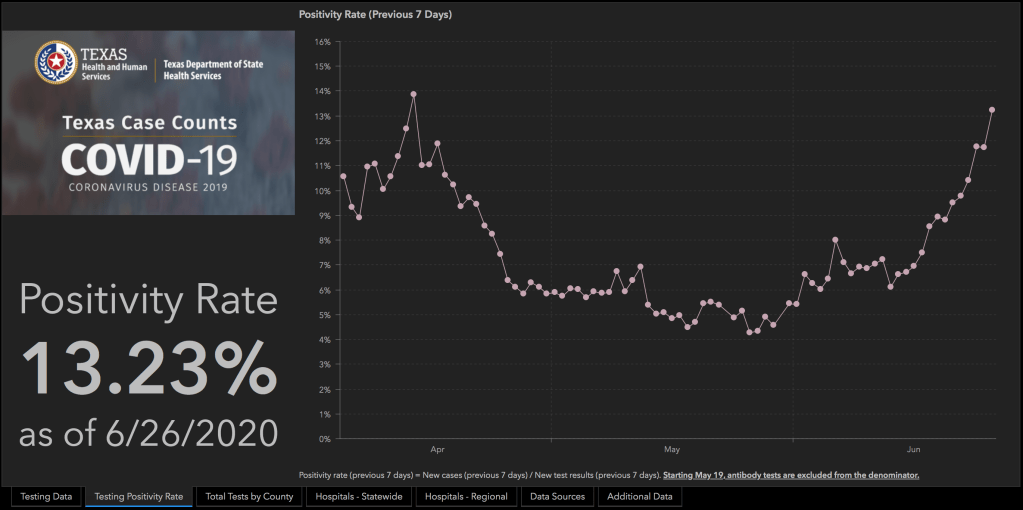
Part 1: Is the rise in cases just due to more testing?
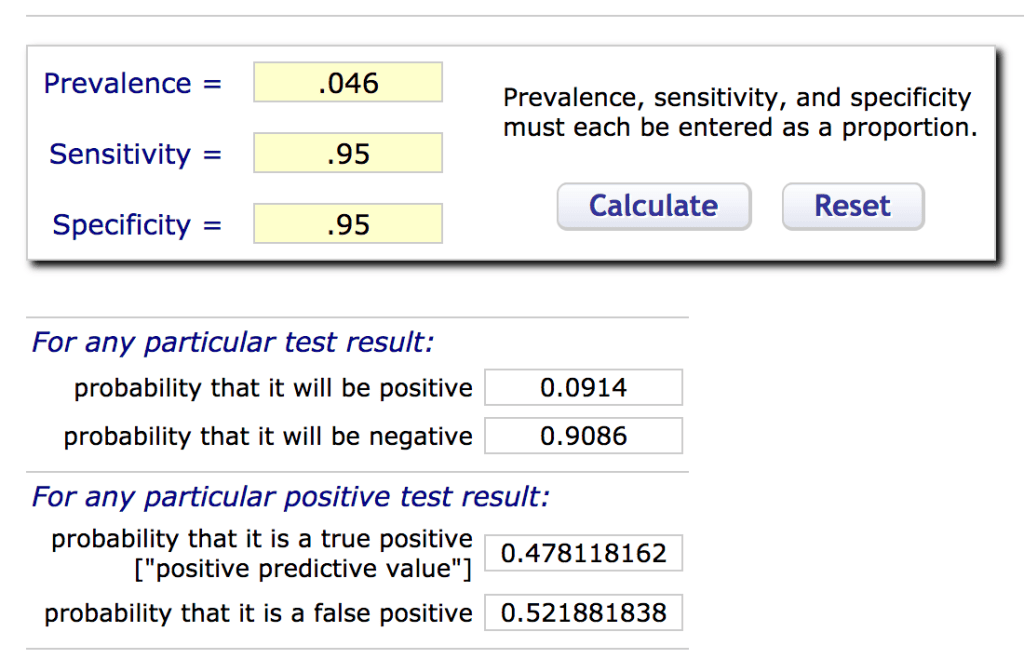
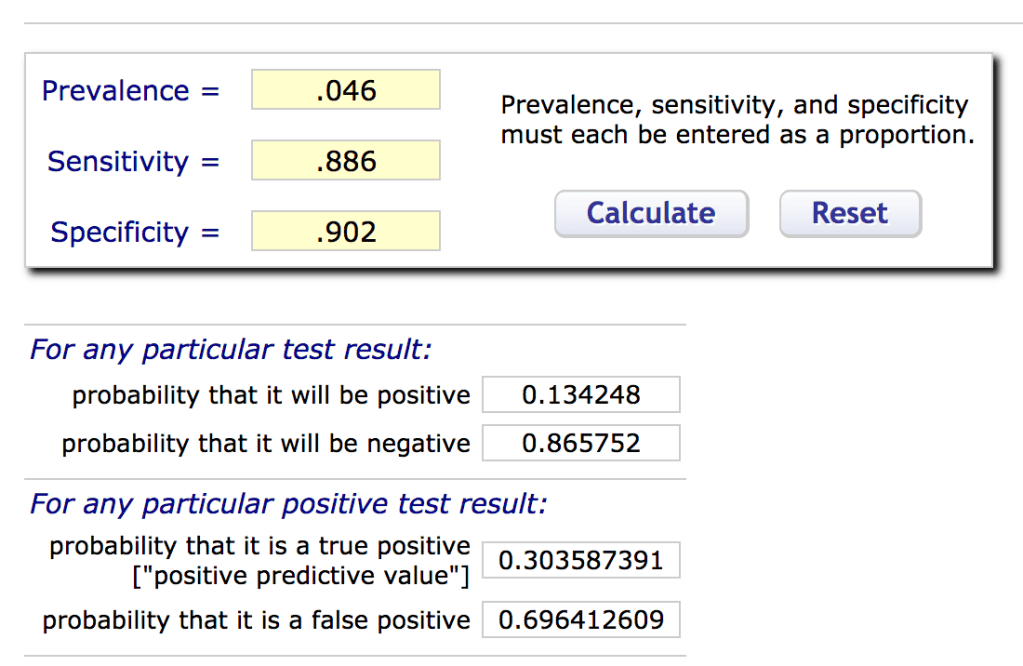
Part 2: What about antibody testing and asymptomatic cases?
Question #3: Isn’t a surge a good thing since it will give us herd immunity?
The concept of herd immunity, susceptible persons being protected from infectious diseases by a sufficiently high number of people in their community already being immune, was controversial even before the COVID-19 pandemic. I don’t mean it was a controversial area of epidemiology; the science behind it is very well established and pretty straightforward (and if you are going to read about the eradication of smallpox from that link, you should also read about a man called Onesimus, a slave in Boston whose knowledge of West African inoculation saved hundreds or thousands of lives and paved the way for Edward Jenner’s eventual invention of vaccination techniques). I mean it was something that we’ve had to argue about constantly in recent years because the anti-vaccine movement uses herd immunity as one of its many arguments against vaccination, while at the same time undercutting its effectiveness by seeking to decrease the number of people who are immune through being vaccinated. The idea is great in principal; just weather the storm now and then we will all be safe from the virus forever. The problem (one of the problems, for there are numerous) is that we don’t yet know exactly what percentage of the population needs to be immune to confer protection to everyone else. Most estimates have put this number somewhere between 60-70%, but a recent model published in Science estimates it at a much more attainable 43%. These numbers are based on several parameters that tell us both how easy the virus is to spread and whether certain activities, situations, or even individuals are more likely to spread it than others (you can read about the median reproduction value and dispersion factor if you want to dive a bit more into the math of it all). Because these numbers are incredibly hard to definitively determine in the midst of a pandemic, any percentage we arrive at is going to be a best guess; an estimate derived from multiple assumptions that will only be proved wrong if many more people get very sick even after we’ve achieved the required numbers for herd immunity. Herd immunity is a gamble because Virology, during a pandemic, is an applied science; the virus will correct all of our miscalculations and false assumptions for us. (other questions, such as whether immunity to SARS-CoV-2 is indeed long-lasting and whether the virus will mutate in such a way that it causes future outbreaks despite our acquired immunity are also important, but outside the immediate scope of the discussion).

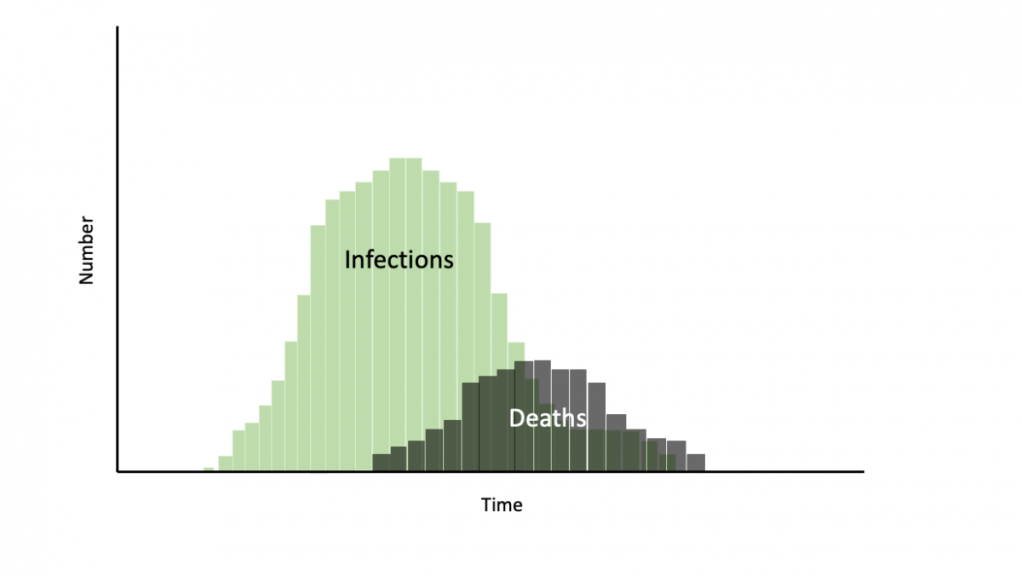
*This is from early in the pandemic, but a great visualization tool
But even more important than the difficulty in calculating the necessary percentage of people being immune to confer protection to everyone else is the question of how dangerous it is to get there in the first place. Let’s talk about measles for one moment. We know that the herd immunity required for measles is somewhere around 93%, which is part of the reason we have seen outbreaks of the disease recently in areas that have a substantial anti-vaccine sub-culture; it isn’t hard to fall below that number. Let’s say there wasn’t a Measles vaccine; that means 93% of people would need to develop immunity by living through the disease. With modern medical advances the case fatality rate for measles is a lot lower than it used to be, but it is still around 2.2%. This means that in a country of 330 million people that had no immunity to measles, 306 million would need to contract the disease to confer herd immunity to everyone else; of those, 6.75 million would die, not to mention the longstanding residual neurological deficits and other health complications in tens of millions more. Without effective vaccination, herd immunity would simply never have been an option for Measles; the cost in human life and suffering would just be too high. But what about COVID-19? We know that SARS-CoV-2 is thankfully less contagious, and we believe less deadly (see the last post for a discussion on this) than measles, but is it enough to make herd immunity a viable option? Let’s apply those same calculations based on the current estimates we have for infection fatality rate. If we accepted a 1% death rate estimate, then to achieve the widely accepted 60% mark for herd immunity we would see 198 million cases and 2 million deaths, while if we accepted the recently released 43% estimate and assumed an even more conservative 0.5% death rate, that would be 709,500 deaths; and neither accounts for the longstanding health deficits or the cost in human suffering of those who survive, or the other deaths and suffering that come with an overwhelmed mid-surge healthcare system. Now, could we devise some clever epidemiology strategy that uses emerging data about the already-immune, super-spreaders, natural resistance, new drug therapies, contact tracing, and protection of the most vulnerable? Of course; assuming that we could get a high degree of buy-in (we can’t even get people to wear masks), that’s exactly what we are all hoping for. But that’s not ‘herd immunity’, and it’s clear that the cost in lives and suffering from a “just get it and get it over with” ‘strategy’ would be astronomical even with our most optimistic estimates. Trust me, I’m tired too; I completely understand the pull towards a roll the dice approach that just gets this over with and lets the chips fall where they may; that approach completely appeals to my intellectual and emotional fatigue. But the longer we can work together to flatten the curve, the more time we create to discover those new therapies, improve our understanding of the virus, and collect high quality data about transmission and vulnerability that can help us develop novel, strategic mitigation approaches (which would probably incorporate something like herd immunity); and we are already seeing the benefits of the work of this kind that we have done so far as a society.
Question #4: What is the RECOVERY Trial?
(Confession: nobody asked about this, but I’m going to write about it anyway)

The RECOVERY Trial is a randomized (poor British researchers spelled it wrong) clinical trial out of Oxford that has shown benefits from using low-dose dexamethasone (a cheap and readily available steroid) for hospitalized COVID-19 patients on oxygen or on a ventilator; you can read a more detailed analysis of the trial from First10EM. This is still in the peer review process but results have been incredibly promising; the study showed a relative decrease in mortality of 20% in hospitalized patients requiring oxygen, and up to a 35% decrease in patients requiring ventilator support. Unlike many of the drug therapies that have been touted up until now, this is based on a randomized trial and not on anecdotal evidence, so it is much more likely that these results will be reproducible when used broadly. Already this has become the standard of care in the hospitals in your city, and if we see these results persist with widespread use it has the potential to save tens or hundreds of thousands of lives. I wanted to write about it for two reasons. First, I want to call on us all now to not let this become the next hydroxychloroquine. The study has established the benefits of this drug therapy only in a specific group of people; hospitalized patients requiring oxygen or ventilator support. They also studied hospitalized patients who were not sick enough to need oxygen, and it showed no benefits whatsoever. There is no reason to infer that this medication is protective in those without severe symptoms or in asymptomatic individuals, and so there is no reason for individuals to ask their doctor for an outpatient prescription or for pharmacies or clinicians to stockpile the medication as we saw done with hydroxychloroquine. We can be thankful that we have at least one helpful medication for our sickest patients without that immediately translating into figuring out a way to get it for ourselves whether it would actually help us or not. And if peer review and follow-up studies and the increased clinical experience that comes with widespread use of dexamethasone ultimately shows that it actually isn’t helpful for COVID-19, that will be tragic; but we should all understand now that that is just how science works, and won’t be part of some big government conspiracy to prevent people from getting the medication, just as it wasn’t with hydroxychloroquine.
But even more importantly, I wanted to talk about the RECOVERY Trial because it illustrates exactly what it looks like to fight this virus by engaging in mitigation and flattening the curve. Since April people have been saying (and we have all been feeling, to some degree or another) that if a certain amount of death and suffering from the virus is inevitable, we might as well just get it over with. We have also heard the slightly more sophisticated position that as long as our hospitals aren’t overwhelmed and we aren’t running out of ventilators and other equipment and resources for sick patients, then we have reduced the danger as much as is helpful and anything more is unnecessary. The RECOVERY Trial is a powerful illustration of why flattening the curve is beneficial even beyond these important goals. If you had a severe case of COVID-19 one month ago and had to be on a ventilator, you would have been treated with hydroxychloroquine and not with dexamethasone; today, you would be treated with dex and not with hydroxychloroquine, and your chance of dying would be 35% less; and that doesn’t even take into account the less quantifiable benefits from all that your doctors have learned about this virus in the meantime. A month from now, with more high quality trials and more clinical experience, who knows what the new standard of care will be and how much better a very sick person’s odds of surviving the virus will be because of it. The reason I wear my PPE with every patient and am a stickler about fomites and transmission, the reason I wear my mask when I’m in public, and the reason I am writing from home instead of a coffee shop today and attended church online this morning, isn’t because I’m afraid of the virus; it’s because when and if (and for me it has always felt more like an ‘if’ than a ‘when’) I get COVID-19, I would rather be treated by doctors and nurses and respiratory therapists who have had ample time to learn how to fight it, who have perfected their approach to ventilator settings and other supportive techniques for this virus specifically, and who have access to medications that have been carefully studied and have been proven to be effective; and because I would like to have that knowledge base and those techniques and medications available if and when I have to treat you.